Insights
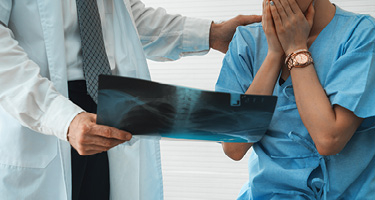
Presenting the 2024 Best Lawyers Employment and Workers’ Compensation Legal Guide
by Best Lawyers
The 2024 Best Lawyers Employment and Workers' Compensation Legal Guide provides exclusive access to all Best Lawyers awards in related practice areas. Read below and explore the legal guide.
Read Full Article

Presenting The Best Lawyers in Australia™ 2025
by Best Lawyers
Best Lawyers is proud to present The Best Lawyers in Australia for 2025, marking the 17th consecutive year of Best Lawyers awards in Australia.
The 2024 Best Lawyers in Spain™
by Best Lawyers
Best Lawyers is honored to announce the 16th edition of The Best Lawyers in Spain™ and the third edition of Best Lawyers: Ones to Watch in Spain™ for 2024.

Best Lawyers Expands Chilean 2024 Awards
by Best Lawyers
Best Lawyers is pleased to announce the 14th edition of The Best Lawyers in Chile™ and the inaugural edition of Best Lawyers: Ones to Watch in Chile™, honoring the top lawyers and firms conferred on by their Chilean peers.

Best Lawyers Expands 2024 Brazilian Awards
by Best Lawyers
Best Lawyers is honored to announce the 14th edition of The Best Lawyers in Brazil™ and the first edition of Best Lawyers: Ones to Watch in Brazil™.

Announcing The Best Lawyers in South Africa™ 2024
by Best Lawyers
Best Lawyers is excited to announce the landmark 15th edition of The Best Lawyers in South Africa™ for 2024, including the exclusive "Law Firm of the Year" awards.

The Best Lawyers in Mexico Celebrates a Milestone Year
by Best Lawyers
Best Lawyers is excited to announce the 15th edition of The Best Lawyers in Mexico™ and the second edition of Best Lawyers: Ones to Watch in Mexico™ for 2024.

How Palworld Is Testing the Limits of Nintendo’s Legal Power
by Gregory Sirico
Many are calling the new game Palworld “Pokémon GO with guns,” noting the games striking similarities. Experts speculate how Nintendo could take legal action.

The Best Lawyers in Portugal™ 2024
by Best Lawyers
The 2024 awards for Portugal include the 14th edition of The Best Lawyers in Portugal™ and 2nd edition of Best Lawyers: Ones to Watch in Portugal™.

How To Find A Pro Bono Lawyer
by Best Lawyers
Best Lawyers dives into the vital role pro bono lawyers play in ensuring access to justice for all and the transformative impact they have on communities.

The Best Lawyers in Peru™ 2024
by Best Lawyers
Best Lawyers is excited to announce the landmark 10th edition of The Best Lawyers in Peru, the prestigious award recognizing the country's lop legal talent.

Presenting the 2024 Best Lawyers Family Law Legal Guide
by Best Lawyers
The 2024 Best Lawyers Family Law Legal Guide is now live and includes recognitions for all Best Lawyers family law awards. Read below and explore the legal guide.

Announcing The Best Lawyers in New Zealand™ 2025 Awards
by Best Lawyers
Best Lawyers is announcing the 16th edition of The Best Lawyers in New Zealand for 2025, including individual Best Lawyers and "Lawyer of the Year" awards.

The Best Lawyers in Colombia™ 2024
by Best Lawyers
Best Lawyers is honored to announce the 14th edition of The Best Lawyers in Colombia™ for 2024, which honors Colombia's most esteemed lawyers and law firms.

Announcing The Best Lawyers in Japan™ 2025
by Best Lawyers
For a milestone 15th edition, Best Lawyers is proud to announce The Best Lawyers in Japan.

How Maine’s Yellow Flag Law Stacks up Against Other New England Gun Restrictions
by Gregory Sirico
New England states currently boast some of the lowest firearm mortality rates in the nation and world, but the state laws of the region vary quite drastically.

Why Backlinks Matter for Law Firm SEO
by Nancy Lippincott
The key ingredient to a law firm's online search visibility could lie within backlinks, a driving factor in the industry's efforts to build an SEO-based future.

Maximizing SEO: The Power of Online Directories for Law Firms
by Nancy Lippincott
By harnessing the power of online directories, law firms can boost SEO, strategically enhancing visibility and overall digital presence in the legal industry.

The Critical Role of Content in Law Firm SEO Strategy
by Nancy Lippincott
From building trust to staying competitive with thought leadership, explore how SEO content creation establishes authority in a largely digital landscape.

Announcing The Best Lawyers in Japan™ 2025
by Best Lawyers
For a milestone 15th edition, Best Lawyers is proud to announce The Best Lawyers in Japan.

The Best Lawyers in Singapore™ 2025 Edition
by Best Lawyers
For 2025, Best Lawyers presents the most esteemed awards for lawyers and law firms in Singapore.

Presenting The Best Lawyers in Australia™ 2025
by Best Lawyers
Best Lawyers is proud to present The Best Lawyers in Australia for 2025, marking the 17th consecutive year of Best Lawyers awards in Australia.

Announcing The Best Lawyers in New Zealand™ 2025 Awards
by Best Lawyers
Best Lawyers is announcing the 16th edition of The Best Lawyers in New Zealand for 2025, including individual Best Lawyers and "Lawyer of the Year" awards.

Connecticut Attorney General Releases Status Update on Data Privacy Act
by Gregory Sirico
Connecticut's attorney general recently released a report on the current status of the Data Privacy Act, focusing in on some keys areas of enforcement.

Colorado Attorney General Calls For Cannabis Reclassification
by Gregory Sirico
In this article, Best Lawyers highlights a recent call to action by the Colorado state attorney general, requesting a full drug reclassification of cannabis.

The U.S. Best Lawyers Voting Season Is Open
by Best Lawyers
The voting season for the 31st edition of The Best Lawyers in America® and the 5th edition of Best Lawyers: Ones to Watch® in America is officially underway, and we are offering some helpful advice to this year’s voters.

IN PARTNERSHIP
Does Your Law Firm Need a COO?
by Esquire Bank
Esquire Bank explains how having a chief operating officer can help with law firm growth plans, business management, client acquisition and daily operations.

IN PARTNERSHIP
Contingency Fee Law Firm Valuation: What Factors Matter for Financing?
by Esquire Bank
Esquire Bank offers information on the valuation of a contingency law firm and the financing options they offer to support law firm growth strategies.

IN PARTNERSHIP
The No-Stress Way to Efficiently Fund a Law Firm
by Esquire Bank
Esquire Bank explains how many lawyers who are starting their own firms can identify a strategic banking partner to offset the difficulties of self-funding.

IN PARTNERSHIP
Should I Hire a Lawyer After a Car Accident in Lawrenceville?
by Yari D. Lawson
If you or a loved one have suffered from a crash, here’s why hiring a car accident lawyer in Lawrenceville, GA, is a good idea to ensure you get compensation.

IN PARTNERSHIP
Protecting Patients and the Public
by Justin Smulison
Lubin & Meyer completes its most successful year yet, charting new territory with a historic class action suit involving hundreds of patients in New England.

IN PARTNERSHIP
Protecting Patients, Families and the Public
by Justin Smulison
Thousands of patients experience unfathomable pain while being treated. Some turn to Koskoff Koskoff & Bieder PC for justice, empathic counsel and results.

IN PARTNERSHIP
Ontario Personal Injury Claims: How Long Can Clients Expect to Wait?
by Salvatore Grillo
Personal injury lawyer Salvatore Grillo discusses types of personal injury claims and how long lawyers and clients can anticipate wait times for resolution.

IN PARTNERSHIP
What Are the Benefits of Hiring a Lawyer After a Car Accident?
by Jamie S. Cogburn
Want to learn more about the benefits of hiring a car accident lawyer? Contact J. Cogburn Law for a free consultation with a Las Vegas car accident lawyer.

IN PARTNERSHIP
Injured in a Car Accident? 7 Steps You Need To Take Immediately
by Mark H. Perenich
Personal injury lawyer Mark Perenich offers advice on the seven most important steps to take immediately after you have been injured in a car accident.

An Employer’s Guidebook to Responding to Online Harassment
by Belle Harris and Brent Siler
Navigating online defamation against your business requires strategic responses. Two employment lawyers guide how to leverage contracts, understand social media limitations and the risks of legal action.

IN PARTNERSHIP
Gust Rosenfeld P.L.C. on Protecting Arizona Employers
by Justin Smulison
Gust Rosenfeld attorney Robert D. Haws discusses emerging trends in employment litigation and how the firm’s Employment and Education Law practice groups have protected clients in and out of Arizona’s courtrooms.

IN PARTNERSHIP
Businesses Must Prepare for the New Department of Labor Independent Contractor Rule
by Kirby Black and Steven T. Clark
Two employment law lawyers explain how a new DOL rule making it more likely workers will be classified as employees, rather than independent contractors, has caused legal challenges and prompted businesses to reassess worker status and policies.

IN PARTNERSHIP
The Wagner Law Group: ERISA and Employment Law
by The Wagner Law Group
For more than 25 years, The Wagner Law Group has combined the personalized attention and reasonable rates of small law firms with the specialization and sophistication of large firms to tackle all of their clients' ERISA and Employment Law needs.

IN PARTNERSHIP
The Long, Short, Thick and Thin of It
by Avrohom Gefen
“Appearance discrimination” based on employees’ height and weight is the latest hot-button issue in employment law. Here’s a guide to avoid discrimination.

IN PARTNERSHIP
5 Things To Do if You’re at Fault in a Car Accident
by Alex De Castroverde
Have you been in a car accident in Las Vegas, NV? Learn more about what to do if you were at fault. Contact a car accident attorney to discuss your case.